New Mom and Pregnancy Packet
When it comes to life, we deliver.

At GRMC, we believe in helping moms be as prepared a possible when it comes to the birth of a new baby. That is why we have created New Mom Packets for all the information you could need and more!
Guadalupe Regional Medical Center offers diagnostic capabilities for high-risk obstetrical patients. GRMC’s services are in association with the University of Texas Health Science Center San Antonio. This partnership enables our local physicians to provide state-of-the-art obstetric and medical care with the latest diagnostic testing.
Outpatient Services provided include:
- Advanced ultrasound / Prenatal diagnosis
- Counseling
- First trimester screening
- Amniocentesis (genetic testing)
- Management of medical complications in pregnancy
Location:
1339 E. Court Street
Suite 230
Seguin, TX 78155
Office Hours and Appointments:
Perinatal Specialists see patients Wednesday mornings. Appointments are scheduled through your OB/GYN physician. You may contact the GRMC MFM Coordinator at 830.401.7195.
Whether you’re expecting your first child or looking forward to another, it’s the special touches that will make your baby’s birth memorable. GRMC’s new Maternity Services Department is now open and combines state-of-the-art technology with spacious and luxurious private rooms and amenities. Our Maternity Services floor has large labor and delivery rooms and dedicated C-section suites that allow our experienced physicians, specially-trained nurses and support staff to provide mother and baby with expert medical care and emotional support during labor, birth and postpartum stay.
When making a decision where your baby will be delivered, you may be wondering how to finance the birth of your child. While GRMC accepts most major insurances, we also understand that maternity care may not be covered. Therefore, GRMC is pleased to announce a new, discounted “Maternity Services Pricing Plan” for families without maternity or traditional health insurance coverage. Qualified, uninsured families may be eligible for this “Maternity Services Pricing Plan” if payment is made in full by the time of the mother’s discharge.
This plan is designed for a normal, uncomplicated delivery at GRMC and for the routine care mother and baby receives during hospitalization. These discounted prices are not offered to families with Medicaid or other maternity insurance coverage. Any special amenities or accommodations may be subject to additional fees.
Please note: There may be other charges depending on the length of your stay, multiple births, or other services you may request. If your baby needs a higher level of care or additional services, additional financial arrangements can be made. The special Maternity Services Pricing does not include physician fees (obstetrician, family practice, pediatrician, neonatologist, anesthesiologists, or radiologist).
Special maternity services pricing:
- Vaginal Delivery – $2800 (2 day stay); $800 per day* thereafter
- Tubal Ligation during a Vaginal Delivery stay: $1400 (in addition to the $2800 VD charge)
- Cesarean Section Delivery – $4200 (3 day stay); $800 per day* thereafter
- Tubal Ligation with Cesarean Section: included with C-section price.
*A day is defined as staying past midnight. The daily rate is limited to a max of 5 days. For stays past 5 days, additional financial arrangements can be made.
You may pay your package rate in either one lump sum or on a payment plan as long as the total is paid in full by the time of your discharge. If not paid in full, by discharge, the special rate no longer applies.
Payments may be made by cash, check or MasterCard/Visa. If your baby must remain in our care for longer than you are here, then those fees are due at the time of discharge. If you pre-pay for a vaginal delivery and require a Cesarean section, you will be asked to pay the difference (noted above) prior to your discharge. Please contact GRMC’s financial counselor at 830.401.7445, for additional questions about this program or to set up a program package.
GRMC’s Birthing Center is focused on mom and baby care throughout your pregnancy. The Birthing Center offers two educational classes; breastfeeding and childbirth. After speaking with your physician about signing up for a class, please contact GRMC’s Birthing Center at 830.401.7530. All Classes are held in the Conference Room next to our Cascades Café.
Learn More about Birthing Center Classes
GRMC also offers a gestational diabetes class focused on complications for the mother, such as preeclampsia and eclampsia, as well as the baby. Examples of focuses include hypoglycemia, hyperinsulinemia, pre-term and respiratory distress, as well as jaundice.
Class topics include:
- What is gestational diabetes and the risk factors for gestational diabetes
- Treatment of gestational diabetes: medications healthy eating, physical activity, monitoring your blood sugar levels
- How to reduce the risk of complication to mother and baby
For more information or to sign up, contact Ann Camacho, 830.484.4237 or acamacho@grmedcenter.com.
One of the most exhilarating and worthwhile experiences of your life will be the birth of your child. Your obstetrician, anesthesiologist and nurses want to help you, the baby and your partner through this event as safely and pleasantly as possible. Every woman has her own unique labor experience. The amount of pain felt will vary for each woman. It depends on factors such as pain tolerance, size and position of the baby, strength of the uterine contractions and prior birth experiences. Decisions about regulating labor pain must be specific to each woman. Some woman can achieve adequate pain control with the breathing and relaxation techniques learned at child birthing classes but others do not. Many woman are reconsidering the idea that a “natural” childbirth can only be achieved if they suffer through without medication and are choosing pain relief for a more comfortable experience.
Choices for pain relief during labor & delivery
Be assured that your physicians will prescribe or administer medications only in the amounts and during those stages of labor that are best for the safety and well-being of your baby. There are several choices for pain relief:
- Intravenous “I.V.” Medication– Pain relieving medications that are injected into a vein or muscle that will help dull you pain but may not eliminate it completely. These I.V. medications are usually prescribed by your obstetrician. Because they sometimes make both you and your baby feel sleepy, they are used mainly during early labor.
- Local Anesthesia– Other pain relieving medications may be injected in the vaginal and rectal areas by your obstetrician at the time of delivery. These medications are local anesthetics. They provide a numbness or loss of sensation in a small area. Local anesthesia is often used to ease the pain of delivery or when an episiotomy incision is done to assist the delivery. It does not, however, lessen the pain of contractions.
- Epidural Blocks– This block can reduce the discomfort of labor. They are administered in the lower back by an anesthesia provider. Local anesthetics and either drugs are used for these procedures to reduce pain and other sensations to the lower body. Epidurals may be used for labor and delivery and/or cesarean deliveries.
- Subarachnoid Blocks– “spinal” may be used for cesarean delivery.
Regional blocks for labor
Labor and delivery epidurals are increasingly popular because they provide for a more comfortable experience. The epidural block has the ability to desensitize the lower areas of the body while leaving the patient conscious. When to administer the epidural block for each patient will vary. If you request an epidural block, the obstetrician and anesthesiologist will evaluate you and your baby’s health, the progress of labor, and the baby’s responses and past anesthetic experiences to determine your individual situation.
Questions & Answers
Q: How is the epidural block performed?
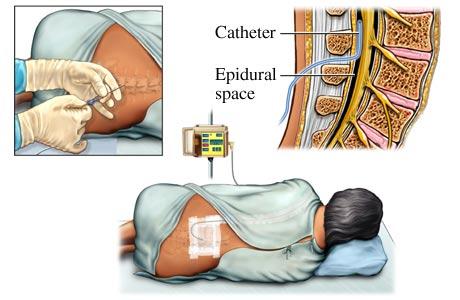
A: The epidural block is administered in the lower back below the level of spinal cord. It is given while the patient is either sitting up or laying to the side. The block could also be given in the tailbone area called a caudal block. First, the skin will be cleansed with an antiseptic solution. The anesthesiologist will then use local anesthesia to numb the area near the tailbone on the lower part of the back. The block is performed with a special needle being placed in the epidural space outside the spinal sac. An epidural catheter, a tiny flexible tube, is inserted through the needle. Occasionally, the catheter touches a nerve sending brief tingling sensations down one leg. When the catheter is situated, the needle is removed and the catheter is taped in place. This process allows for additional medications to be given throughout the experience and allows continual pain blocking as the nerves are numbed. This produce sepidural analgesia.
Q: How soon will the epidural block take?
A: The onset of pain relief with an epidural block is gradual because it needs to be absorbed into several nerves. The effect will take within 10-20 min after being injected to numb the area
Q: What will I feel after the block takes effect?
A: Considerable pain relief will occur, but pressure or sensations from contractions may still be noticeable. Some women feel the obstetrician’s examinations as labor progresses. Depending on each mother and baby’s circumstances, the anesthesiologist adjusts the numbness for comfort and to assist labor and delivery. Some woman even notice a degree of temporary numbness, heaviness or weakness in their legs.
Q: How long will the block last?
A: The epidural analgesia can be extended for as long as you need it. Once the epidural catheter is in place, additional medication can be administered as needed. An anesthesiologist and nurse will monitor your comfort and progress throughout your labor and adjust medications accordingly. After delivery, the catheter is removed and sensations return to normal within a few hours.
Q: Will the epidural affect my baby?
A: Research has shown that both mother and baby can be safe with the use of epidural analgesia and anesthesia with little to no effect on the infant. However, a qualified anesthesiologist should perform this procedure because of the importance of special medical training and judgment, precautions and treatments involved.
Q: Will it slow down my labor?
A: Epidural medications have various effects on different people. Some mothers may feel a brief period of decreased uterine contractions. Many, however, are pleasantly surprised to learn that once the epidural medications have relaxed them, they are more comfortable and their labor actually can progress faster.
Q: Can I “push” when needed?
A: Epidurals allow you to rest during the longest part of labor, which occurs during cervical dilation.
Q: When is general anesthesia used?
A: General anesthesia is used when a regional block is not possible or is not the best choice for medical or other reasons. It can be started instantaneously and causes a rapid loss of consciousness. This is the procedure used when an urgent vaginal or cesarean delivery is required, as in rare instances of problems with the baby or vaginal bleeding. In these circumstances, general anesthesia is quite safe for the baby. The main concern during general anesthesia is if there is food or liquids in the mother’s stomach. During unconsciousness, “aspiration” can occur, meaning that some stomach contents come up and go into the lungs. In the lungs, they could possibly cause pneumonia. Anesthesiologists take extra precautions to protect the lungs, such as placing a breathing tube in the mouth and windpipe after anesthetized. Before a cesarean delivery, the mother may be given and antacid to neutralize the stomach acid. Remember, DON’T EAT OR DRINK ANYTHING AFTER LABOR PAINS BEGIN, regardless of delivery plans or pain control. Sometimes during labor, small sips of water, clear liquids or ice chips are permissible with the physician’s consent.
Q: Will I receive a separate bill from the anesthesiologist?
A: An anesthesiologist is a physician specialist like an obstetrician or pediatrician whose medical services have been requested. It is probable that a separate bill will be received specifically for the anesthesiologist’s professional service as would be true for other physicians. If you have any financial concerns, your anesthesiologist or an office staff member will answer your questions. Note that your hospital charges separately for medications and equipment used.
Options
Modern anesthesiology offers today’s mother’s a variety of options for more comfortable childbirth. The anesthesiologists’ goal is to answer questions, ease fears and make the labor and delivery experience as safe as possible for your baby. Please discuss any anesthesia-related questions or concerns with your obstetrician. Usually, a consultation with an anesthesiologist can be arranged before your delivery. The more prepared you are –in other words, the more time spent “planning for the childbirth” – the more comfortable and memorable the birth of your baby will be!
Birthing Ball
GRMC has two birthing balls available for use.
Peanut Ball
GRMC has two peanut balls available for use. This will help mom by opening up her hips and allowing baby to progress to birth canal.
Patterned Breathing
Breathing techniques provide comfort and focus while enhancing labor progress.
Movement and Position Changes
Moving about during labor is usually more comfortable than staying still and can help labor progress by the simple effects of gravity and the changing shape of the pelvis.
Superficial Heat and Cold
Heat can be effective when applied by using hot moist towels, or warm blankets. While cold can come from an ice bag or washcloths soaked in ice water.
Counter-Pressure
Steady, strong force applied to one spot on the lower back during contractions. This helps alleviate back pain during labor, especially in those women experiencing “back labor”.
Touch and Massage
Touch or massages can convey pain-reducing messages.
Aromatherapy
Aromatherapy is the use of essential oils such as lavender, rose, chamomile, and sage.
Focus and Distraction
Methods of coping with pain rely on the ability to focus and use mind-diverting activities.
Audio-Analgesia
Music creates a peaceful and relaxing environment and aids in relaxation. Carefully chosen music can also reinforce rhythmic breathing patterns.
Our Birthing Center offers a beautiful, brand new 4 bed triage for outpatient care. The triage area is utilized for screening patients for labor status, as well as caring for patients that are here for outpatient obstetric care prior to being in labor. The triage area has direct access to our Birthing Center unit, as well as our operating rooms, should your status require you to be admitted for the delivery of your baby.
Upon arrival to the triage area, you will be greeted by a highly qualified Registered Nurse (RN) and shown to a private bed. Your RN will be in contact with your obstetrician to assure that you receive the best care possible.
 The Birthing Center are GRMC has been nationally recognized by Healthgrades as being a 5-Star Recipient for vaginal delivery care 6 years in a row! We are honored that GRMC’s Birthing Center has been acknowledged on a national level and we continue to make it our goal to provide a family-centered environment that delivers a safe and pleasant childbirth experience!
The Birthing Center are GRMC has been nationally recognized by Healthgrades as being a 5-Star Recipient for vaginal delivery care 6 years in a row! We are honored that GRMC’s Birthing Center has been acknowledged on a national level and we continue to make it our goal to provide a family-centered environment that delivers a safe and pleasant childbirth experience!
At GRMC, our goal is to provide you with a family birthing center that delivers a safe and pleasant childbirth experience. While delivering your baby at our Birthing Center, you can expect:
- A welcoming and relaxing environment in our waiting room
- Experienced staff providing you support and education as you progress in labor
- Highly skilled nurses monitoring your labor and keeping your physician informed of your progress
- Family Centered Care – meaning we keep your baby with you as often as possible
- Strong lactation support, including skin to skin for parents and baby
- Expert team to care for your baby
- And much more
We also offer two OR C-Section Suites, which are located inside the Birthing Center, so you are always in close proximity to an operating room should you need a c-section. You can feel at ease knowing that you will keep the same nursing staff during your c-section that you had while in the Birthing Center.
We highly encourage your baby to stay with you during your time at our Birthing Center and encourage you to hold your baby, skin-to-skin, throughout your time here. Babies kept near their mother tend to feed and sleep better, cry less, and overall remain healthier. Additionally, keeping your baby with you will allow you to learn your babies cues and help you feel more confident when going home.
If your baby needs special care or treatment, our Neonatologist offers the high level care you are looking for. The Birthing Center at GRMC is equipped with advanced technology to care for your newborn. Our Neonatologist works closely with you in planning developmentally appropriate care based on your baby’s needs.
Our Birthing Center is equipped with a state of the art Continuing Care Nursery. Should your baby require additional support at birth, we have a separate 2 bed Continuing Care Nursery where they will be cared for by our highly skilled nursing staff as well as our in-house Neonatologist or one of our Pediatricians.
We understand the importance of bonding with your newborn and should your newborn need to stay for continuing care, we will offer you the option of a complimentary stay in your room after discharge so that you can be close to them at all times.
Local Pediatricians and Family Practice experts are ready to provide immediate care following birth and throughout childhood. All of the outstanding specialists below are accepting new patients.

Susan Boullioun, MD
Family Practice
113 E. Cedar St.
Seguin, TX 78155
830.303.3500

Brett Earnest, MD*
Family Practice
1761 South, TX-46, Suite 104
New Braunfels, TX 78130
830.433.7815

Michele Lopez-Glynn, MD*
Pediatrics
1005 E. Court St.
Seguin, TX 78155
830.303.3400

Whitney Morgan, MD
Pediatrics
515 N. King St., Suite 101
Seguin, TX 78155
830.372.3135

James Rider, MD
Family Practice
1414 E. Walnut St.
Seguin, TX 78155
830.379.7901

Esther Robbins, MD
Family Practice
411 S. King St.
Seguin, TX 78155
830.433.7030

Phillip Rinn, MD
Family Practice
519 N. King St.
Seguin, TX 78155
830.372.0994

Robert Stephens, MD
Pediatrics
520 E. Donegan St.
Seguin, TX 78155
830.379.6300

Nicole Talbot, DO
Family Practice
515 N. King St.
Seguin, TX 78155
830.372.5200
*Denotes Accepts Medicaid
